[This is a media release from the Robert Wood Johnson Foundation.]
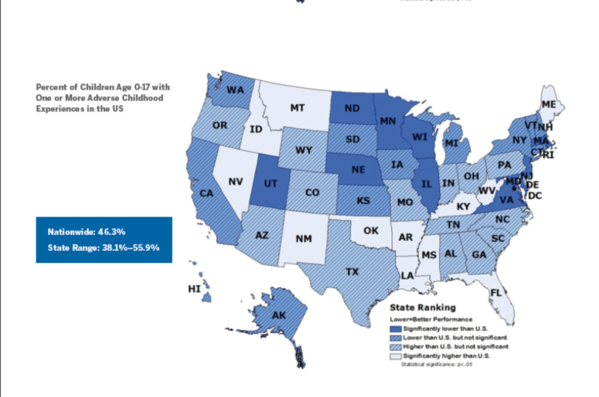
New national data show that at least 38 percent of children in every state have had at least one Adverse Childhood Experience or ACE, such as the death or incarceration of a parent, witnessing or being a victim of violence, or living with someone who has been suicidal or had a drug or alcohol problem. In 16 states, at least 25 percent of children have had two or more ACEs. Findings come from data in the 2016 National Survey of Children’s Health and an analysis conducted by the Child & Adolescent Health Measurement Initiative (CAHMI) at the Johns Hopkins Bloomberg School of Public Health, and are being released by the Robert Wood Johnson Foundation (RWJF) in collaboration with CAHMI.
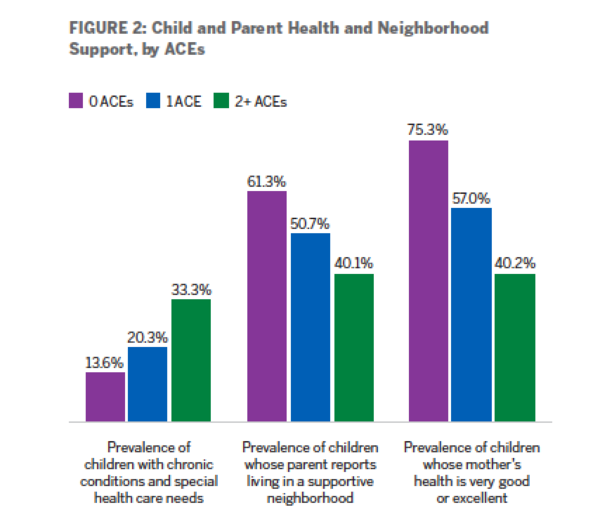
ACEs can have serious, long-term impacts on a child’s health and well-being by contributing to high levels of toxic stress that derail healthy physical, social, emotional, and cognitive development. Research shows that ACEs increase the long-term risk for smoking, alcoholism, depression, heart and liver diseases, and dozens of other illnesses and unhealthy behaviors. The new data show that 33 percent of children with two or more ACEs have a chronic health condition involving a special health care need, compared to 13.6 percent of children without ACEs.
Nationally, more than 46 percent of U.S. youth—34 million children under age 18—have had at least one ACE, and more than 20 percent have had at least two. The new analysis includes state-by-state percentages of children with ACEs, ranging from 38.1 percent in Minnesota to 55.9 percent in Arkansas. The ten states with the highest rates are either in the South or West. The newest national and state data, along with an issue brief and maps, can be found at www.cahmi.org.
“Every child deserves a healthy start. A loving home, a good school, a safe neighborhood—these things are the foundation for a long and happy life, yet too many children don’t have them,” said Richard Besser, president and CEO of the Robert Wood Johnson Foundation. “Too often children experience trauma that can be devastating. But trauma doesn’t have to define a child’s life trajectory. They can be incredibly resilient. With policies that help families raise healthy children, and the consistent presence of caring adults in their lives, we can reduce the impact of trauma on children’s health and help them thrive in the face of adversity.”
Key findings from the new data analysis include:
ACEs impact children and families across racial, ethnic, and socioeconomic groups.
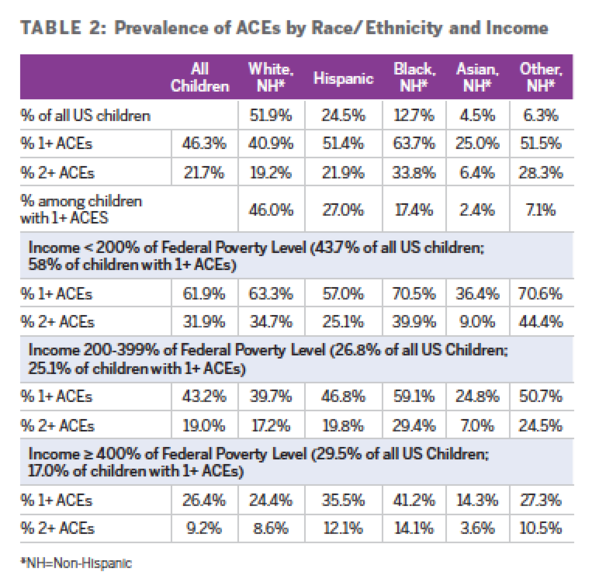
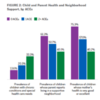
- White children are less likely to have ACEs than Hispanic or Black children, but they make up the plurality of all children who have had ACEs. Roughly 40 percent of white children have one or more ACEs, compared to 51 percent of Hispanic children and nearly 64 percent of black children. But in part because of demographics, 46 percent of children who have had one or more ACEs are White, whereas 27 percent are Hispanic and 17 percent are Black.
- ACEs are more prevalent among children in low-income families—62 percent of children with family incomes under 200 percent of the federal poverty level have had at least one ACEs. But they occur among children at all income levels—26 percent of children in families with incomes higher than 400 percent of the federal poverty level have had one or more ACEs as well.
ACEs impact a child’s social emotional development and chances of school success.
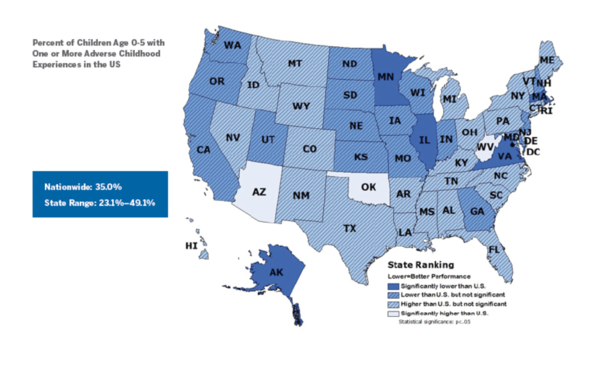
- Children ages 3-5 who have had two or more ACEs are over four times more likely to have three out of six social and emotional challenges, for example, have trouble calming themselves down, be easily distracted, and have a hard time making and keeping friends.
- More than three out of four children ages 3-5 who have been expelled from preschool also had ACEs.
- Children ages 6-17 who have had two or more ACEs are twice as likely to be disengaged from school than are peers who have had no ACEs.
Supportive relationships and teaching resilience skills can mitigate the effects of ACEs.
- Children ages 6-17 who have had two or more ACEs but learned to stay calm and in control when faced with challenges are over three times more likely to be engaged in school compared to peers who have not learned these skills.
- Children whose parents report “always” having positive communication with their child’s health care providers are over 1.5 times more likely to have family routines and habits that can protect against ACEs, such as eating family meals together, reading to children, limiting screen time and not using tobacco at home.
“ACEs and other traumatic events don’t just affect an individual child—families, neighborhoods and communities all bear the brunt of these difficult circumstances, which add up over time,” said Dr. Christina Bethell, director of CAHMI. “If a child’s stress and unhealed trauma leads to acting out in class, that disruption is felt by the other children in the room as well as the teacher. These impacts require the healing of trauma at a family, community, and societal level. Practitioners and policymakers should respond to these new data by advancing strategies that can both prevent ACEs in the first place and support families and communities as they learn and heal.”
Attached is a document -- ChildrenACEs.pdf - that contains more data, including state data.
The Robert Wood Johnson Foundation supports a range of policies to help prevent ACEs from occurring, and help families respond to them, including:
- Policies like paid family leave and home visiting to ensure that parents and caregivers have the time, knowledge, and resources they need to support their children.
- Policies that can improve access to and the quality of child care and early education
- Policies that can help create healthier communities such as those focused on safe affordable housing, access to healthy foods and community violence prevention.
Last month, CAHMI and AcademyHealth published a special supplement to the journal Academic Pediatrics which collected a wide array of research on ACEs and put forth the first-ever national agenda to address ACEs and promote resilience, healing, and child and family well-being. The agenda emphasized that supportive community policies can help reduce the trauma caused by ACEs.
The National Survey of Children’s Health (NSCH) is funded and directed by the Maternal and Child Health Bureau (MCHB), which develops survey content in collaboration with a national technical expert panel, and the U.S. Census Bureau. The NSCH first included questions about ACEs in the 2011/12 survey, but the methods and sample size changed between then and 2016, meaning it is not advisable to directly compare results across years. Plans are for the NSCH to be an annual survey so that data trends can be evaluated. The ACEs assessed in the survey are:
- Somewhat often/very often hard to get by on income
- Parent/guardian divorced or separated
- Parent/guardian died
- Parent/guardian served time in jail
- Saw or heard violence in the home
- Victim of violence or witness violence in neighborhood
- Lived with anyone mentally ill, suicidal, or depressed
- Lived with anyone with alcohol or drug problem
- Often treated or judged unfairly due to race/ethnicity
_______________________________
For more than 40 years the Robert Wood Johnson Foundation has worked to improve health and health care. We are striving to build a national Culture of Health that will enable all to live longer, healthier lives now and for generations to come. For more information, visit www.rwjf.org. Follow the Foundation on Twitter at www.rwjf.org/twitter or on Facebook at www.rwjf.org/facebook.
About the Child and Adolescent Health Measurement Initiative
The Child and Adolescent Health Measurement Initiative (CAHMI) promotes early and lifelong health of children, youth and families by developing and advancing actionable use of family-centered data, measures, research and engagement tools (www.cahmi.org). The CAHMI was founded in 1997 and is based out of the Bloomberg School of Public Health at Johns Hopkins University in Baltimore, Maryland. CAHMI partnered with RWJF, AcademyHealth and the Children’s Hospital Association to study rates and impacts of ACEs using the 2016 NSCH. CAHMI works with the federal Maternal and Child Health Bureau in the design of the NSCH and analyzes and publishes state by state findings on its interactive data query accessible on the Data Resource Center for Child and Adolescent Health website, www.childhealthdata.org. Follow CAHMI on Twitter at @CAHMI2Thrive or on Facebook www.facebook.com/childhealthdata.





Comments (4)