Many of us don’t fully appreciate how too little or poor quality sleep affects mood, brain function, and brain health. Improving sleep is particularly important for survivors of adverse childhood experiences (ACEs), for whom disturbed sleep is common.
Too Little Sleep
Experts now recommend 7-9 hours of sleep nightly for most adults. Sleep shortage, particularly less than six hours per night, is a stressor linked to higher risks for:
- Psychological problems—such as anxiety; depression; poorer memory, concentration, and decision making; worsening of PTSD symptoms; cognitive decline; and Alzheimer’s disease
- Physical problems—such as fatigue, pain, weight gain, plaque buildup in the arteries, heart attack, stroke, irregular heartbeat, high blood pressure, autoimmune disorders, kidney problems, diabetes, cancer, and death from all causes
- Inflammation—which might contribute to most, if not all, all of the conditions mentioned above. There is a vicious cycle between sleep shortage, obesity and inflammation. Sleep shortage leads to weight gain, perhaps because people become too tired to exercise and because sleep shortage causes the release of hormones that increase hunger and promote snacking. Fat cells then release inflammatory chemicals, which cause or worsen many conditions that interfere with good sleep.
Benefits of Good Sleep
- Good sleep reduces the risk for the conditions noted above. For example, good sleepers on average are leaner and snack less at night.
- Adequate sleep allows cerebrospinal fluid to flow between brain neurons and wash away toxins and junk proteins, like the beta-amyloid proteins that form plaques in Alzheimer’s disease. This is a possible reason why good sleepers are less likely to develop dementia.
- Good sleepers are even much more likely to forgive.
Recommendations
1.Treat nightmares. Repetitive nightmares, which disturb sleep, are common in ACEs survivors. Nightmares signal a need to process and settle disturbing memory material. Imagery rehearsal training (IRT) has been found to improve nightmare frequency, PTSD symptoms, and sleep quality.
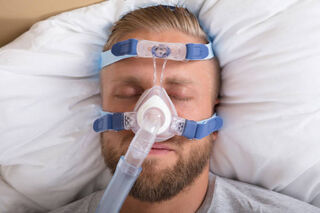
2. Treat obstructive sleep apnea (OSA). About 10% of adults have OSA. It is common in people with PTSD and depression or who are overweight. OSA occurs when muscles of the upper airway relax during sleep and the airways collapse. Breathing stops from seconds to a minute or more and people partially and repeatedly wake up to get oxygen to the lungs. Oxygen deprivation can lead to next-day fatigue, sluggishness, concentration problems, headaches, and sexual disinterest. OSA is a serious risk for nightmares, depression, high blood pressure, heart attack, stroke, diabetes, accumulation of plaques associated with Alzheimer’s disease, and smaller volume in brain areas important in memory. OSA is also linked to chronic inflammation. Treatment frequently improves symptoms of PTSD and depression—and the other symptoms and risks mentioned above. Fortunately, apnea is very treatable. Treating apnea has been found to improve PTSD treatment outcomes. Talk to your doctor about diagnosing apnea with a sleep study or a home sleep test. The gold standard for treatment is continuous positive airway pressure (CPAP). An oral appliance and surgery are other treatment options.
3. Treat insomnia symptoms with cognitive behavioral therapy for insomnia (CBT-I), which is considered the gold standard and first-line treatment for insomnia. CBT-I not only improves insomnia, but also lowers the risk of developing depression in older adults. It is more effective in the long run than sleep medications, it has no side effects, and benefits persist after treatment ends. CBT-I helps people: eliminate arousing thoughts about sleep; relax; implement sleep hygiene practices (see below); track sleep patterns; and restrict sleep (which shortens time in bed to increase the drive to sleep and then gradually lengthens sleep duration). CBT-I can be administered by a trained professional in person, by telephone, through internet-based programs (with or without professional support), and even by self-help books.
The Department of Veterans Affairs has developed a free online app called CBT-i Coach that anyone can use, either to augment needed in-person therapy or use on it’s own. Also see the VA Path to Better Sleep course (https://tinyurl.com/VACBTI). Other online options, such as SHUTi and Sleepio, usually costing $150 or less, may be covered by insurance.
4. Worry efficiently. People who wrote about their worries—the facts, thoughts, and feelings—for 25 minutes a day significantly reduced the worry and anxiety that was keeping them awake at night. Find a neutral place to write about your worries (not your bed). During the day, postpone your worries until your worry period.
Sleep Hygiene
These practices are generally helpful to improve sleep quality and duration.
- Keep a consistent sleep schedule—go to bed and get up at the same times, even on weekends, to help the brain maintain daily sleep rhythms. Consistency reduces the risk of drowsiness, insomnia, headaches, mood swings, memory and other brain dysfunctions, stroke, and heart attack.
- Wind down. At least an hour before bedtime, shut off screens, which emit blue light. Blue light suppresses the release of melatonin, which promotes sleepiness. If your electronics have a night mode setting, use it toward the end of the day to limit blue light. Instead of screen time, relax with a good book, soothing music, or other calming activities.
- Try a warm bath or shower about ninety minutes before bedtime. Water at about 104 degrees Fahrenheit has been found to help people fall asleep faster and improve sleep quality. In response to the heat, the body cools down, which promotes good sleep. A cool room temperature also helps to regulate body temperature.
- Eat a light dinner, but not within four hours of going to bed. Digestion can override the tendency to sleep. Cut back on liquids after dinner. If low blood sugar wakes you up at night, try a light snack near bedtime (such as warm milk and honey).
- Morning exercise in the sun helps to regulate the sleep cycle. For good sleepers, evening exercise at least 2 hours before bedtime is better than none. Yoga, tai chi, and meditation might also improve sleep.
- Limit caffeine, nicotine, and alcohol. Alcohol, for example, helps people fall asleep, but then acts as a stimulant and diuretic later on, causing you to wake up and need to use the bathroom. Alcohol also relaxes muscles in the throat, causing or worsening apnea. If used, limit caffeinated drinks to the morning.
- Nap? Maybe, but not too long or late. About 60% of people benefit from napping (such as more successful aging and improved memory and learning). The best time is before 3:00 pm, when there is a natural circadian dip. Keep naps under thirty minutes to avoid grogginess and interference with nighttime sleep. Long naps might signal poor sleep at night from depression, diabetes, thyroid disorders, or other health problems that need treatment. If you have insomnia, avoid napping in order to consolidate nighttime sleep.
- Supplements? Perhaps. There is little evidence that valerian, GABA, kava, or herb supplements improve sleep. However, ashwagandha might help you sleep by reducing stress, anxiety, and cortisol levels (this should not be used by those who are pregnant or nursing, or who have an autoimmune or thyroid disease). Two or more servings of fatty fish weekly or fish oil supplements (with 1000 mg of EPA and DHA omega-3s taken daily) have anti-inflammatory and analgesic properties, and may help you sleep. Check with your doctor before trying supplements.
- Only use prescription and over-the-counter sleep aids with caution. Sleeping pill use can result in dependence, tolerance, rebound insomnia, worsening of apnea, and next-day impairment. Benzodiazepine use has been linked to dementia.
Antihistamines are anticholinergic drugs, meaning they block acetylcholine—a major neurotransmitter in the brain. Antihistamine use causes or exacerbates cognitive impairment and brain aging. Antihistamines are found in Sominex, Unisom, pain relievers like Tylenol PM and Advil PM, and cold remedies like Nyquil. Remember that non-pharmacological strategies usually work as well or better than medications, without side effects.
Conclusion
As we age, it is normal to find it more challenging to get a good night’s sleep. However, it’s comforting to know that these strategies can improve the odds of optimizing brain health and function—preparing it to rewire negative neural pathways imprinted by ACEs.
In the next blog we’ll explore managing nightmares in more depth.
Reference
Schiraldi, G. R. (2021). The Adverse Childhood Experiences Recovery Workbook. Oakland, CA: New Harbinger.
This article also appeared in Psychology Today.
About the Author
Glenn R. Schiraldi, PhD, has served on the stress management faculties at The Pentagon, the International Critical Incident Stress Foundation, and the University of Maryland, where he received the Outstanding Teacher Award in addition to other teaching/service awards. His fourteen books on stress-related topics have been translated into seventeen languages, and include The Adverse Childhood Experiences Recovery Workbook, The Self-Esteem Workbook. The Resilience Workbook, and The Post-Traumatic Stress Disorder Sourcebook. The founder of Resilience Training International (www.ResilienceFirst.com), he has trained laypersons, emergency responders, and clinicians around the world on the diverse aspects of stress, trauma, and resilience.
Photo Credits
Adene Sanchez/istockphoto; yinyang/istockphoto; AndreyPopov/istockphoto






Comments (0)