Dr. Elisa Nicholas, a pediatrician and chief executive officer of TCC Family Health Clinics in Long Beach, California, relays an example of how the COVID-19 pandemic has wreaked havoc on the lives of the clinics’ patients. Most had already been struggling financially prior to the pandemic.
“Both the mother and father came down with coronavirus,” said Nicholas. “Their child was in on a telephone visit with one of our doctors. They did not have any way to get food. They had no money to pay for two months of rent [that they owed], and they were going to be evicted from the trailer park where they were living.
“We brought them food immediately, provided them with grocery vouchers for food delivery, and paid their rent,” she said.
She said the clinics were able to use money from a Mental Health Services Act grant that allowed them to shift some funds to address immediate, concrete concerns. Nicholas says that with the growing risk of hunger among families they serve, the clinics have set up food pantries on site.
Nicholas was one of several speakers participating in an ACEs Connection webinar on Aug. 27 to talk about the fallout from the COVID-19 pandemic and the social unrest following the killing of George Floyd, as well as opportunities to push for policies that prevent and mitigate childhood trauma. The webinar was organized by the California Campaign to Counter Childhood Adversity (4CA), made up of more than 100 organizations, including TCC Family Health. 4CA was founded by the Center for Youth Wellness. CYW, Children Now and ACEs Connection serve as core facilitators for 4CA.
Nicholas and her colleagues have been in emergency mode ever since the pandemic hit in March. At that time, she directed staff to set up tents outside for visits and testing and made sure TCC Family Health Clinics' seven clinics could serve its 40,000 patients at a safe social distance. They also initiated a mask-making effort and looked for indoor locations to house the population it serves that was already homeless.
Through it all, Nicholas was seriously concerned about the safety of the clinics’ staff. “The struggle for us has been [having enough] personal protective equipment,” she said.
At the moment, AB 2537 passed the Senate on Aug. 30. and SB 275 is making its way through the state legislature, calling for health care providers to have between a 45-day and three-month supply of personal protective equipment on hand. But Nicholas says that goal may be hard to meet, given the hierarchy of distribution that puts hospitals at the top of the totem pole and community clinics like hers down lower.
“We're all jockeying for the same PPE, which is ridiculous,” she said.
Testing for COVID-19 also has run into roadblocks. “Every day, about 75 patients come in with signs or symptoms of COVID,” said Nicholas. At first, the clinics simply didn’t have the supplies to do testing. Then the supplies arrived, but there was a significant delay in getting test results.
“So the doctors in our clinics were saying, ‘Why should I test someone if we're not going to get the results for 17 days?’” she said.
Nicholas is hoping that some recently awarded federal funding will help speed up test results.
About 24 percent of patients at the clinics have tested positive, and there have been at least two deaths. Nicholas believes that overcrowding in poor families has contributed to the problem. “We’ve had a lot of cases go through entire families,” she said.
While patients have been hit hard, so has the TCC staff. About half of the TCC Family Health Clinics’ 440 employees have been out sick, and many have had to stay home for other reasons.
“One of the big issues facing us now is that our essential employees do not have childcare,” Nicholas explained. “So we have doctors who aren’t working because they're having to work on educating their kids, and a lot of our line staff are struggling. Some aren’t working, and if they are, they're going home and having to do a lot of the [school] work with their kids.”
While supplies and testing have been riddled with problems, federal approval to reimburse health care providers for remote visits with patients has resulted in a dramatic uptick in the number of people getting support.
“We've had almost a 100% [attendance] rate in our behavioral health visits through telephonic visits, which is incredible because usually the behavioral health visits are very low,” Nicholas said. “And if you want to address childhood trauma, you want to make access to behavioral health as barrier-free as possible.”
The problem is that federal approval for remote visits is given only on an emergency basis, which worries Nicholas greatly. “If it ends, it will destabilize the community health centers,” she said.
Nicholas noted that she and others are in conversation with state health officials and legislators to push for long-term coverage of remote visits, and she encouraged others participating in the webinar to join that effort.
Nicholas is also concerned about promoting what she calls “tech equity” among her patients, and she’s working with a local legislator to help get Wi-Fi to families that don’t have it at home. They need to be able to connect with their health care providers, she explained, and have access to other remote tools, such as blood pressure monitoring devices.
Lynnan Svensson, the public health nursing manager in El Dorado County, California, was the next speaker at the webinar. She summed up the toll that the COVID-19 pandemic has taken on her agency: “We have way too many competing priorities, so what's happening is organizational trauma. Our workforce was burned out even before COVID.”
She links the internal burnout to years of underfunding. “We had really severe budget cuts back in 2008 and 2009 that we’ve never recovered from,” she said. Politics often dictates which sectors get funding. “In most counties, law enforcement gets most of the funding, while public health gets very little,” she noted.
Those cuts gutted her workforce; El Dorado County lost two-thirds of its employees. And because of burnout, some employees are choosing to retire or leave the profession altogether. That means that most public health workers who remain have to put in seven-day work weeks, primarily to deal with COVID-19.
Those efforts include educating a largely conservative and resistant populace about why they need to wear masks. When necessary, Svensson said, she dons her “sticker badge” and closes down gatherings of recalcitrant residents.
She and her colleagues are also involved in public health announcements to keep people up-to-date on the ever-changing recommendations, and they’re helping to stave off outbreaks in nursing homes, jails and hospitals through testing and contact tracing. As a result, many other much-needed programs that serve vulnerable populations, such as maternal, child, and adolescent health, and disability and communicable-disease prevention, are falling by the wayside.
Another challenge is building trust and making COVID-awareness inroads among the Latinx population, which is the second-largest demographic in the county, after Whites. “There was already distrust of the government and fear of deportation,” Svensson said. Those fears are now compounded by basic survival issues, she adds, “like having to work when they're sick.”
In the midst of all of this, Svensson and her colleagues were thrown another curve ball in late August, when the California wildfires forced many families to evacuate their homes.
And to top it off, Svensson, like others on the front line, has family matters of her own that need attention. “My parents are failing. I need to move them up here to my home in Northern California. My husband's out of a job due to COVID, and my daughter is in her last year of nursing school, which is stressful.”
Recently, Svensson said, the state has provided more funding for her agency, which she plans to use to beef up her depleted staff. She’s grateful, but hopes that it’s more than just a one-off. It’s time that politics are removed from public health funding, she said, “because this won’t be the only infectious disease or emergency issue that public health needs to lead on.”
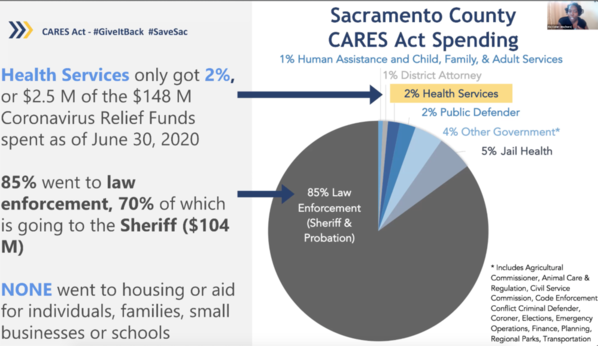
Dr. Flojaune Cofer, the senior director of policy for Public Health Advocates, said county decisions about the distribution of federal COVID-19 funds could exacerbate health inequities. A clear example, she said, is the way Sacramento County distributed the Congressional funding it received through the CARES Act.
“We learned about two weeks ago that health services got 2% of the money, while the remainder went to law enforcement,” she said. “Seventy percent went to the sheriff. I’m furious about what has actually happened with these dollars!”
Cofer brought up problems with the funding on a recent call with U.S. Senator Kamala Harris, the Democratic vice-presidential nominee.
Cofer points to other areas of need during the pandemic that have been neglected. “We have almost 100,000 households that are either behind on rent or unable to pay [altogether]," she said. "So to contrast that with giving most of the money to law enforcement is really, really challenging.”
A particularly scandalous part of the funding discrepancy, Cofer said, is the way Sacramento County supervisors responded when they were called on it.
“They said everyone got what they needed," she said. "And our county public health director went on the record and said, ‘That's a baldfaced lie. We asked for $90 million.’”
But the most galling exchange for Cofer was one that clearly showed how profoundly county officials don’t understand what things are like on the ground.
“One of the county supervisors said to our county public health officer, ‘Well, when they told you you couldn’t get what you needed, why didn’t you fight more?’ I wanted to throw things and curse,” Cofer said. “Because if you think about what Lynnan and Elisa just described, we’re talking about COVID-19. We’re talking about fires. We’re talking about extreme heat here in the area of 112 degrees during the day — all at the same time. And you want to ask why I can’t fight for more money?”
To listen to the full recording of the webinar, including the questions and answers, check back here for a link, which will likely be available in the next week.


Comments (0)