The United States is on the threshold of advancing much needed improvements in child and population well-being by addressing the epidemic of adverse childhood experiences and finding ways to come together, use what we know, and heal and catalyze a new epidemic of child and family flourishing.
A special issue of Academic Pediatrics highlights new national research with inspiring commentaries across a wide range of leaders, each of whom calls out the critical importance of an immediate, strong and collective policy response; and the critical roles for Medicaid and private sector health plans, children’s hospitals, primary care providers and all children’s health services as key partners with families and communities. Science-driven methods to proactively promote resilience and healthy relationships is central to mitigate the far-reaching consequences of ACEs for children, families and communities.
The journal issue sets forth a collectively developed action agenda to promote the possible — flourishing for all — by healing the effects of current and accumulated individual, intergenerational, systems and community-level ACEs.
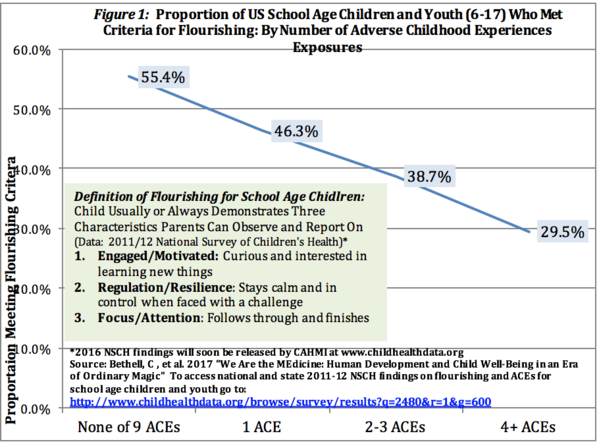
Recent data show that nearly half of American children – 35 million kids – had at least one adverse childhood experience (ACE). Fewer than two in five children flourish when they have had two or more of these experiences; these
include abuse, neglect, divorce, incarceration of a parent or traumas in their communities through exposure to poverty, violence, and disease. Wide variation in the impact of ACEs and evidence of what we can do point to the urgent need to promote healthy parenting, teach resilience, address systems change so that organizations stop traumatizing already traumatized people, and address social and economic inequities impacting family and community capacity to heal and prevent ACEs.
The collection of papers sends a clarion call for the public and policymakers to understand that ACEs can have devastating, long-lasting neurobiological and psychosocial effects on children’s health and well-being that resonate well beyond the individual child to have far-reaching consequences for families, neighborhoods, organizations, systems, communities and society.
Some of the policy priorities and recommendations for action include:
- Translating the science of ACEs, cultivating policies to enable effective collaboration across sectors, fuel “launch and learn” initiatives to support innovation and real-time learning, and reward outcomes that support safe, stable and nurturing relationships centered around activating and supporting individual, family, organization, system and community self-care, prevention and healing.
- Capitalizing on short-term policy opportunities, such as maintaining the nation’s EPSDT program that prioritizes early screening, testing and prevention, as well as leveraging existing policy systems, practice transformation efforts, and research and data platforms.
Overall the agenda lays out what I call a “We Are the Medicine” approach that points to the necessity and power of each of us and all organizations in society to be a part of the solution. The relational wounding represented by ACEs requires relational healing, and in this way every interaction matters — we matter and how we are with one another moment by moment can impact each other profoundly. As we all learn about ACEs and learn the skills to attune and relate mindfully and in ways that promote safety, trust and authentic sharing, we go a long way to heal the neurobiological and psychosocial impacts that ACEs can lead to and that are leading our society into a crisis.
Several articles focus on positive relationships with service providers, within medical home-based care teams and among community partners as pivotal to the success of efforts to address ACEs and promote flourishing, especially to integrate mental and behavioral health into clinical care. Related to this, a critical and common theme called out across several papers was the need for providers and leaders to develop their own self-awareness about ACEs and engage in active self-care to be able to offer a healing presence and authentically engage children, youth and families to discuss ACEs and promote flourishing. What I have called this "Your Being, Their Well-Being" mandate is something to begin now.
Also included in the special journal issue is a commentary on how promoting child well-being and addressing ACEs aligns with the Robert Wood Johnson Foundation’s Culture of Health framework, which seeks to engage all sectors to improve population health, well-being, and equity. Other articles address frameworks for addressing and measuring ACEs, priorities and practices for systems of care and clinicians, community and family approaches to preventing or responding to ACEs, and related policy implications.
Key steps to develop the national agenda and the publication of the September issue of Academic Pediatrics were funded by the Robert Wood Johnson Foundation and led by the Child and Adolescent Health Measurement Initiative at the Johns Hopkins Bloomberg School of Public Health and AcademyHealth.
To learn more about this special issue of Academic Pediatrics please contact me at cbethell@jhu.edu. Follow the discussion on Twitter: @CAHMI2Thrive and at @AcademyHealth.
NOTE: Publication of this journal issue of Academic Pediatrics is commensurate with the release of selected findings from the 2016 National Survey of Children’s Health. Early results show variations in system performance and health of women, children and youth by ACEs and flourishing status of children. More extensive findings from the 2016 NSCH will released in the fall (www.childhealthdata.org). Access national and state child flourishing and ACEs data here.
Links to Academic Pediatrics’ ACEs special issue:
Overall – 1
Foreward – 2
Commentaries – 3-17
Articles – 18-31
Summary from National Agenda and Field Building Collaboration – 18
Frameworks and Measurement – 19-22
Systems of Care and Clinical Practice – 23-26
Community and Family Approaches – 27-28
Implications for Policy – 29-31
- Overall Journal Issue: http://www.academicpedsjnl.net...1876-2859(17)X0002-8
- Foreword – Child Well-being and Adverse Childhood Experiences in the United States. Bethell, C.D., Simpson, L.A., & Solloway, M.R. pp. S1-S3: http://www.academicpedsjnl.net...-2859(17)30370-4/pdf
- Promoting Lifelong Health and Well-being: Staying the Course to Promote Health and Prevent the Effects of Adverse Childhood and Community Experiences. Davis, M., Costigan, T., Schubert, K. pp. S4-S6: http://www.academicpedsjnl.net...-2859(16)30532-0/pdf
- Aligning Community Capacity, Networks, and Solutions to Address Adverse Childhood Experiences and Increase Resilience. Hargreaves, M.B., Pecora, P.J., & Williamson, G. pp. S7-S8: http://www.academicpedsjnl.net...-2859(17)30150-X/pdf
- The Community and Public Well-being Model: A New Framework and Graduate Curriculum for Addressing Adverse Childhood Experiences. Ford, D.E. pp. S9-S11: http://www.academicpedsjnl.net...-2859(17)30167-5/pdf
- Reclaiming the Patient Encounter. Hassink, S.G. pp. S12-S13: http://www.academicpedsjnl.net...-2859(16)30411-9/pdf
- Prevent, Screen, Heal: Collective Action to Fight the Toxic Effects of Early Life Adversity. Burke Harris, N., Silvério Marques, S., Oh, D., Bucci, M., & Cloutier, M. pp. S14-S15: http://www.academicpedsjnl.net...-2859(16)30505-8/pdf
- ACEs Implications for Nurses, Nursing Education, and Nursing Practice. Girouard, S. & Bailey, N. pp. S16-S17: http://www.academicpedsjnl.net...-2859(16)30424-7/pdf
- Lessons from ACEs: Pay Now or Pay (More) Later. Grimes, K.E. pp. S18-S19: http://www.academicpedsjnl.net...-2859(16)30554-X/pdf
- “Nothing About Us Without Us.” Vickers, M.C. & Wells, N. pp. S20-S21: http://www.academicpedsjnl.net...-2859(16)30502-2/pdf
- Culture Matters: Direct Service Programs Cannot Solve Widespread, Complex, Intergenerational Social Problems. Culture Change Can. Porter, L., Martin, K., & Anda, R. pp. S22-S23: http://www.academicpedsjnl.net...-2859(16)30496-X/pdf
- Translating Brain Science Research into Community-Level Change. Jones, J., Reidy, M.C., Hargreaves, M., & Rog, D. pp. S24-S25: http://www.academicpedsjnl.net...-2859(16)30423-5/pdf
- How Social Journalism Accelerates the ACEs Movement. Stevens, J. pp. S26-S27: http://www.academicpedsjnl.net...-2859(16)30556-3/pdf
- Mitigating Adverse Childhood Experiences Through Investments in Early Childhood Programs. Beckmann, K.A. pp. S28-S29: http://www.academicpedsjnl.net...-2859(16)30420-X/pdf
- ACEs and State Maternal Child Health Programs. Planey, B. pp. S30-S31: http://www.academicpedsjnl.net...-2859(16)30493-4/pdf
- ACEs and the Criminal Justice System. Garbarino, J. pp. S32-S33: http://www.academicpedsjnl.net...-2859(16)30419-3/pdf
- ACEs and Child Health Policy: The Enduring Case for EPSDT. Rosenbaum, S. pp. S34-S35: http://www.academicpedsjnl.net...-2859(17)30111-0/pdf
- Prioritizing Possibilities for Child and Family Health: An Agenda to Address Adverse Childhood Experiences and Foster the Social and Emotional Roots of Well-being in Pediatrics. Bethell, C.D., Solloway, M.R., Guinosso, S., Hassink, S., Srivastav, A., Ford, D., & Simpson, L.A. pp. S36-S50: http://www.academicpedsjnl.net...-2859(17)30354-6/pdf Supplemental Materials: http://www.academicpedsjnl.net.../2081261501/mmc1.pdf
- Methods to Assess Adverse Childhood Experiences of Children and Families: Toward Approaches to Promote Child Well-being in Policy and Practice. Bethell, C.D., Carle, A., Hudziak, J., Gombojav, N., Powers, K., Wade, R., & Braveman, P. pp. S51-S69: http://www.academicpedsjnl.net...-2859(17)30324-8/pdf
- Income Inequality and the Differential Effect of Adverse Childhood Experiences in US Children. Halfon, N., Larson, K., Son, J., Lu, M., & Bethell, C. pp. S70-S78: http://www.academicpedsjnl.net...-2859(16)30497-1/pdf
- Responding to ACEs With HOPE: Health Outcomes From Positive Experiences. Sege, R.D. & Harper Browne, C. pp. S79-S85: http://www.academicpedsjnl.net...-2859(17)30107-9/pdf
- A New Framework for Addressing Adverse Childhood and Community Experiences: The Building Community Resilience Model. Ellis, W.R. & Dietz, W.H. pp. S86-S93: http://www.academicpedsjnl.net...-2859(16)30552-6/pdf
- The Central Role of Relationships With Trauma-Informed Integrated Care for Children and Youth. Brown, J.D., King, M.A., & Wissow, L.S. pp. S94-S101: http://www.academicpedsjnl.net...-2859(17)30015-3/pdf
- Best Practices in Relational Skills Training for Medical Trainees and Providers: An Essential Element of Addressing Adverse Childhood Experiences and Promoting Resilience. Magen, E. & DeLisser, H.M. pp. S102-S107: http://www.academicpedsjnl.net...-2859(17)30106-7/pdf
- Adverse Childhood Experiences and Resilience: Addressing the Unique Needs of Adolescents. Soleimanpour, S., Geierstanger, S., & Brindis, C.D. pp. S108-S114: http://www.academicpedsjnl.net...-2859(17)30010-4/pdf
- Adapting the Patient-Centered Medical Home to Address Psychosocial Adversity: Results of a Qualitative Study. Vu, C., Rothman, E., Kistin, C.J., Barton, K., Bulman, B., Budzak-Garza, A., Olson-Dorff, D., & Bair-Merritt, M.H. pp. S115-S122: http://www.academicpedsjnl.net...-2859(17)30016-5/pdf
- ACE, Place, Race, and Poverty: Building Hope for Children. Bruner, C. pp. S123-S129: http://www.academicpedsjnl.net...-2859(17)30352-2/pdf
- Developing a Community-Wide Initiative to Address Childhood Adversity and Toxic Stress: A Case Study of The Philadelphia ACE Task Force. Pachter, L.M., Lieberman, L., Bloom, S.L., & Fein, J.A. pp. S130-S135: http://www.academicpedsjnl.net...-2859(17)30168-7/pdf
- Addressing Adverse Childhood Experiences Through the Affordable Care Act: Promising Advances and Missed Opportunities. Srivastav, A., Fairbrother, G., & Simpson, L.A. pp. S136-S143: http://www.academicpedsjnl.net...-2859(17)30163-8/pdf
- Financing Mechanisms for Reducing Adversity and Enhancing Resilience Through Implementation of Primary Prevention. Steverman, S.M. & Shern, D.L. pp. S144-S149: http://www.academicpedsjnl.net...-2859(17)30149-3/pdf
- Evolving a More Nurturing Society to Prevent Adverse Childhood Experiences. Biglan, A., Van Ryzin, M.J., & Hawkins, J.D. pp. S150-S157: http://www.academicpedsjnl.net...-2859(17)30148-1/pdf



Comments (1)