Whether it’s racial profiling at traffic stops or microaggressions at work, racism by any measure can cause toxic stress. That causal relationship and how it leads to a greater burden of ACEs (adverse childhood experiences) among communities of color was the subject of a webinar on April 28 entitled “Racism and Discrimination as Risk Factors for Toxic Stress,” sponsored by the California Surgeon General’s Office and the ACEs Aware Initiative.
“I can't think of a more important conversation to be having right now,” said California Surgeon General Dr. Nadine Burke Harris. “The significance of this issue has come into focus even more sharply in the last year, in the context of a nearly 150% increase in anti-Asian hate crimes, in repeated incidents of police killings of Black men and women, and a disproportionate burden of COVID-19 cases and deaths in communities of color.”
The other speakers at the event included Dr. Aletha Maybank, chief health equity officer for the American Medical Association, and Dr. Ray Bignall, assistant professor of pediatrics at Nationwide Children’s Hospital in Columbus, Ohio.
Burke Harris explained that the original Adverse Childhood Experiences (ACEs) Study and subsequent research that’s emerged from it, tying ACE scores to relative risks for health conditions later in life, did not expressly include racism as an adverse childhood experience.
But the research makes clear, she said, that “Racism and the resulting systemic inequities create conditions that lead to ACEs, such as disproportionate incarceration rates among people of color. And [the Centers for Disease Control and Prevention] data demonstrates that communities of color carry a higher burden of ACEs and are at greater risk of ACEs-associated health conditions.”
Burke Harris also noted that poorer communities and communities of color are often located in areas that lack access to healthy produce, recreational areas and parks and community spaces that buffer toxic stress. “Exposure to racism can act as a direct and chronic stressor,” she said, but she added that there are strategies to help health providers mitigate toxic stress associated with racism in their patients.
To uproot racism, name its cause
In order to develop solutions to racism, you have to be able to clearly name what’s causing it, which is white supremacy, said Maybank, who works with the AMA’s Center for Health Equity. “And we don't talk about that, or name that often enough,” she said. “It's important that we start shifting in that direction, so we can make sure that our solutions are directed where they need to be.”
Another common mistake in trying to in root out racism in institutions is to assign one person or a team to work on it without ensuring there will be a shift in the entire institution, said Maybank. How does that happen?
“Our teams need to understand what equity means in the first place. How does it show up in the day-to-day decisions that they make? And what do they need to do in order to prevent further harm?”
The model that the AMA is using, said Maybank, is based on developing a shared language. “Often the reason why we really can’t have conversations around race, power, privilege, is because we don’t have the same language or understanding,” she said.
To have a shared language, she said, there needs to be training “beyond implicit bias training.” This training should:
- Include structural competencies in anti-racism
- Identify champions
- Develop an accountability system within the institution to ensure action
- Identify tools necessary to challenge existing models on a day-to-day basis
- Set up trauma-informed and healing systems.
It’s also important to build alliances and share power with marginalized and “minoritized” people and communities, Maybank said, going beyond simply having them as members of advisory committees.
“How are we going to develop structures and processes that consistently center the experiences and ideas of historically marginalized people and minorities?” At the AMA, she said, that means international medical graduates, people with disabilities, and Black, Latinx, Asian and LGBTQ physicians.
Another part of the center’s strategy is working with a community-led coalition, such as West Side United in Chicago. “Because we’re engaging with others, it prevents trauma and that typical top-down approach that institutions like the AMA and many others have [used],” she said, “potentially retraumatizing the neighborhoods and the people we’re trying to serve.”
To further support truth, reconciliation and healing, the AMA last fall adopted a policy that calls out racism as a public health threat. This was relatively new for the private health sector but has been a tenet of public health for a while.
She said that institutions like the AMA also must hold themselves accountable for their racist past policies and practices, including the exclusion of Black physicians from membership until the 1960s and its recommendation in 1910 that five of the seven medical schools for Black students be closed.
“So, our work will be to continue to amplify those narratives that are often hidden, and then to quantify how our policies have harmed people and, and to figure out how we’re going to repair and cultivate healing from that harm,” she said.
A staggering impact
Bignall, the pediatrics professor, shifted the discussion from the institutional level to the individual physician. In particular, he focused in on pediatricians and family doctors who are working to prevent and mitigate toxic stress and ACEs in their young patients and in their communities. He said that such work cannot succeed without a clear understanding of how thoroughly racism and systems of inequality permeate every aspect of life.
He pointed to a number of systems of inequality, including redlining, food insecurity, income inequality, education inequality, policing and incarceration, and health inequities. “I believe the research shows that ACEs catalyze these unequal conditions that imperil child health,” he said.
After the Great Depression, Bignall said, President Franklin Delano Roosevelt’s New Deal subsidized American home ownership to help lift Americans out of poverty.
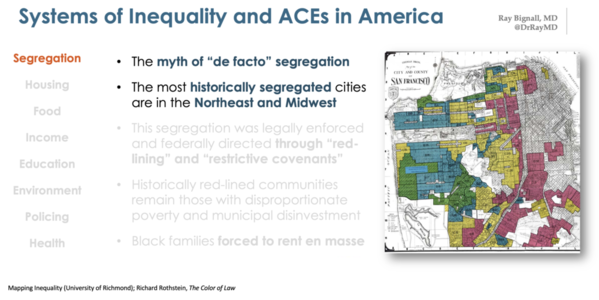
“The federal government brought these lifelines to millions of Americans, but Black Americans were explicitly excluded from this entitlement with devastatingly surgical precision,” he said. As an example, he showed a color-coded map of San Francisco, illustrating which neighborhoods were eligible for investment.
“It was those communities that were historically redlined that remain those disproportionately impoverished today,” he said. “And those same communities, by the way, experience decreased municipal investment, which results in many of the communities in which concentrated ACEs can be found.”
Bignall says the inability to build wealth through home ownership is compounded by higher unemployment among Blacks than whites, and income inequality, with the median income for Black families less than 10 cents for every dollar of wealth for White families.
On top of all these inequities is the disproportionate policing and criminalization of Blacks compared to Whites. Bignall pointed to a national study linking a childhood history of parental incarceration and juvenile justice involvement to mental health issues in early adulthood.
The study found that nearly 1 in 10 children had a history of parental incarceration and 1 in 20 had a history of juvenile justice involvement. The researchers found that children who experienced both parental incarceration and involvement in the juvenile justice system were twice as likely to experience anxiety and three times as likely to experience depression or PTSD than their peers who did not have incarcerated parents or juvenile justice involvement.
“The web of systemic racism, and ACEs and adverse child health captured by this study is truly staggering,” Bignall said. African Americans are nearly six times more likely to be incarcerated than Whites, according to a study by the Sentencing Project.
Bignall, a kidney specialist, points to a study of food insecurity in children on dialysis with kidney failure. The researcher found that while food insecurity affects 20 percent of all households, it affects two-thirds of children with end-stage kidney disease.
“The ability to purchase nutritious foods is incredibly challenging for those families that deal with income inequality and often redlining correlates with ‘food deserts’ that we see in our communities,” he said. “Over-policed neighborhoods are less desirable for investment and less likely to attract supermarkets or fresh food vendors and health care utilizations.” (See this study on how redlining contributes to food deserts in communities of color.)
When Bignall looks at the study through an ACEs lens, he sees more. “Insecure housing can leave many families, including children, at risk for physical, emotional and sexual abuse,” he said. “Tenuous financial circumstances may leave children at risk for abuse and physical neglect as well. Increased carceral and law enforcement exposure can lead to adverse child mental health. And the accumulation of ACEs contributes directly to poor health outcomes.”
Bignall suggests that doctors combine these perspectives into a pediatric visit that can help prevent and mitigate ACEs:
- Consider the child’s mental health, the family’s financial circumstances, and the environment they live in, which could contribute to their illness.
- Screen for ACEs and social determinants of health.
- Have a plan for offering interventions if the screening results are positive.
- Support primary prevention strategies such as paid family leave, high quality education for everyone, and family access to health care.
- Integrate psychologists and mental health providers into health settings. “They can teach patients coping strategies and mindfulness for facing ACEs in their everyday life,” he noted.
- Build community partnerships.
Here’s a link to watch the entire webinar, and here is a link to the slide deck.



Comments (1)